June 21, 2022 Industry news
Late in April 2022, The Faculty of Clinical Informatics (FCI) released a preliminary publication of the new draft Standards and Interoperability Strategy commissioned by the NHS England and Improvement Transformation Directorate.

Titled ‘How Standards Will Support Interoperability’, the strategy outlines a series of objectives intended to promote the interoperability of data across the NHS.
The vision is this: “[To establish] a health and social care system that enables all relevant care information accessible to those who have a legitimate right to do so, at the point of need, wherever it is held”. Achieving system-wide interoperability is the ultimate end goal but, to achieve this, access to standardised data is crucial.
As a global standards organisation, this strategy clearly resonates with GS1 UK as its aims reflect our own – to harness the power of standards to transform the way we work and live.
In healthcare our standards – GS1 standards – are used to uniquely identify every person, every product, and every place throughout the supply chain and patient pathway. In doing so, this allows greater visibility and traceability from manufacturer to patient by using standardised data to enable interoperability.
Where do GS1 standards align?
Universal adoption of the NHS number as the unique patient identifier
Aligns with GS1’s principles of positive patient identification.
At the centre of the architectural approach to interoperability lies the adoption of the NHS number. “Many issues across the NHS have at their root cause the inability for two systems to be able to tell that they want to exchange data for the same patient.”
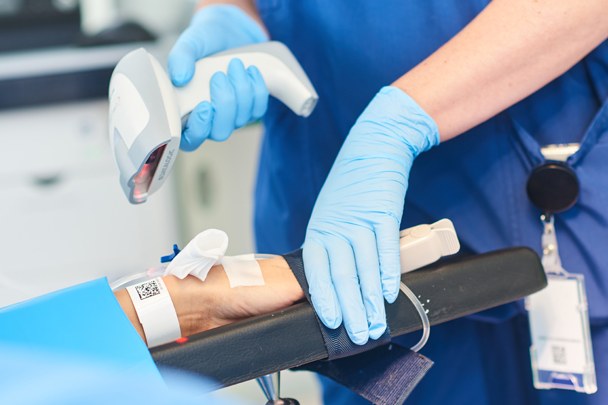
Internal-based system identifiers, such as the medical record number (MRN), are frequently still used as the primary identifier for patients. This is not a problem if there is only one system in use, and in a single organisation, but add another system into the equation or consider a transfer of care request to another healthcare provider and traceability unravels.
An MRN for a patient in one organisation, can easily be attributed separately to a different patient in another location. It has happened before and still happens, sometimes with detrimental consequences.
Recent investigations conducted by The Healthcare Safety Investigation Branch (HSIB) into incorrect patient identification provide clear examples of the implications of patient misidentification.
In these instances, the recommendation is clear – the consistent use of the NHS number. Noting this as a specific national safety risk, the strategy states: ‘The NHS number is a unique identifier for people living in England (and Wales). There is a chance that a patient may be incorrectly identified when the NHS number is not used.’
Additionally, the HSIB makes the following observation: ‘It may be beneficial if further national work is undertaken on the use of the NHS number as a unique identifier, specifically in identifying patients.’
NHS Digital’s standard for automatic identification and data capture (AIDC), DCB1077, already exists for this purpose. In this instance, the NHS number (along with other approved patient identifiers i.e. name, date of birth and sex) is encoded into a 2D GS1 DataMatrix. This information is contained alongside a GS1 globally unique identifier to create the GS1 Global Service Relation Number (GSRN).
By using the GSRN, this provides a globally unique means of identifying patients – not just from one organisation to another, but also from country to country. This supports interoperability requirements for worldwide patient traceability by way of a global shared care record, the International Patient Summary.
The widespread adoption of dm+d
Aligns with GS1’s principles of unique product identification which spans medicines, medical devices, and assets.
The NHS Dictionary of medicines and devices (dm+d) is a universal standard for the standardised capture of production information associated with medicinal products.
“The standard’s primary purpose is to support interoperability. Therefore, electronic systems that exchange or share information about medicines relating directly to a patient’s care must adhere to the standard by using dm+d identifiers and descriptions when transferring information.”

It relies on four key components for standardisation, one of which is the ‘identification of medicines within the supply chain by the inclusion of GS1 GTIN codes where known’.
The GS1 Global Trade Item Number (GTIN) provides an accurate and consistent way of identifying products. Encoded into a 2D GS1 DataMatrix barcode along with relevant production information (such as batch/lot number and expiry date), accurate medicines information can be captured and shared across various relevant systems.
End-to-end traceability
Aligns with GS1’s principles of accurate identification of places for effective location management to enable traceability.
The strategy centres on getting the right data, to the right people, in right place, at the right time. The benefits of doing so are significant – not just to clinical staff, but crucially, to patients.
Six key advantages are highlighted in the strategy:
- Improve the quality of care through access to data e.g. reduce the risk that care is provided based on partial or inaccurate information and reduce medicine prescribing errors
- Release time to care for clinicians by giving them quick and direct access to the information they need
- Reduce the inefficiencies and safety risks of data entry from paper or different systems
- Harness the power of clinical decision support and insights to help optimise care
- People who use services will no longer need to remember specific details of their medical history
- Staff will be able to move from one care setting to another more easily
Using GS1 standards, data can easily be captured at the point of care for every person, product, and place as required. Through point of care barcode scanning, staff gain access to accurate information in real time.
The Scan4Safety report’s findings provide clear evidence to support this.
Headline data from the report include:
- The release of 140,000 hours of clinical time back to patient care
- Reduced prevented-error rates by 76 per cent, including elimination of all errors caused by wrong patient, wrong drug, wrong dose and wrong form at Royal Cornwall Hospitals NHS Trust
- Reduction in the average time taken for product recalls, from 8.33 days to less than 35 minutes at Leeds Teaching Hospitals NHS Trust
- Non-recurrent inventory reductions of £9m across the six demonstrator sites
- Recurrent inventory savings worth nearly £5m across the six trusts

When standardised data is done right
System-wide integration in healthcare cannot be achieved without interoperability, and for this, universal open standards need to be in place. This reflects the main principles of the end-to-end model framework outlined in the draft.
Not only does it make sense to align data for interoperability across the English health system, it also makes sense to do so with globally unique identifiers, ensuring data is fit for purpose, not just now but also in the future. In doing so, international health systems will be equipped for interoperability, promoting full traceability throughout the world.
Make sure the data is unique, accurate, captured once, and shared to many – the benefits are there for the taking. Now is the time to make the most of the potential of standards to enable interoperability and deliver greater continuity of care for patients.



