February 08, 2024 Industry news
HSSIB releases a national learning report following widespread investigations into patient misidentification errors.
The Healthcare Services Safety Investigations Body (HSSIB), formerly the Healthcare Services Investigation Branch (HSIB), is “a fully independent arm’s length body of the Department of Health and Social Care”. The organisation “investigates patient safety concerns across the NHS in England and in independent healthcare settings where safety learning could also help to improve NHS care”.
The national learning report
On 8 February 2024, the HSSIB released a national learning report following widespread investigations into positive patient identification. Aimed “at healthcare organisations and policymakers”, it is designed “to help improve patient safety in relation to patient identification” following reports of several incidents of patient misidentification.
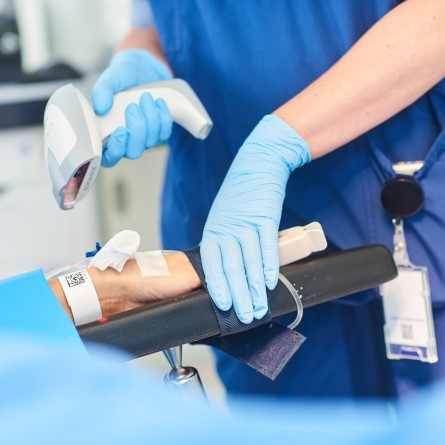
The report highlights the critical importance of unique patient identification, explores how using data standards can be used to minimise identification errors, and how using technologies such as point-of-care barcode scanning improves patient safety.
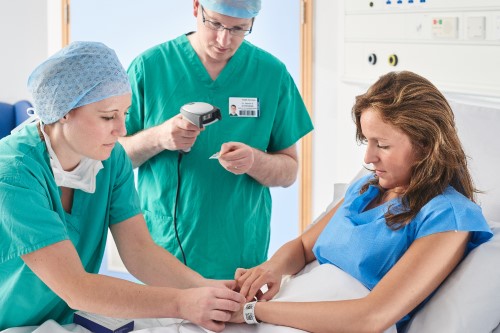
Importance of positive patient identification
In recent years, six full investigative reports into patient misidentification have been conducted by HSIB. These cover instances “where a patient is identified as someone else”, which often lead to the intended patient receiving the incorrect treatment proposed for another.
One such example can be found in the HSIB’s local integrated investigation pilot 1 – incorrect patient identification released in 2021 which refers to patient who was admitted to hospital under another patient’s NHS number. Patient care was given under another patient’s identity before the error was picked up on day seven of admission.
National standards for accurate positive patient identification
In the report, the HSSIB states “to support patient identification in England, the patient’s NHS number should be used alongside other identifiers, such as their name, date of birth and address”.
NHS England data standards DCB1077, DAPB0108, and ISB0099, are mandatory standards in place to ensure the accurate unique identification of patients. These standards work in tandem to make sure patient identifiers are captured in a standardised format that can be used nationally.
The standard DCB1077: AIDC for Patient Identification, “supports the accurate, timely and safer identification of NHS patients in England by using barcodes for positive patient identification”. It defines “how to encode the NHS approved patient identifiers into the GS1 DataMatrix barcode (a two-dimensional barcode) and covers production, verification and printing rules for the barcode”.
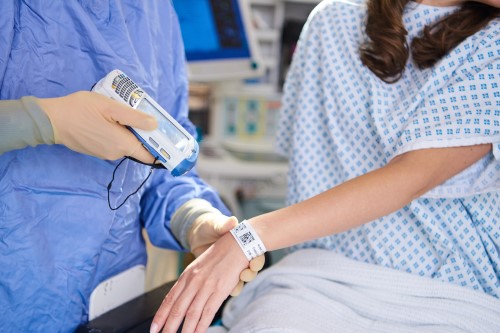
DCB1077 uses the GS1 Global Service Relation Number (GSRN) – a globally unique identification number – alongside the NHS number and patient identifiable information, to significantly reduce the risk of incorrect patient identification.
All NHS trusts in England that have implemented, or intend to implement, Automatic Identification and Data Capture (AIDC) must adhere to DCB1077 requirements for compliance. This is intended for use alongside the standards DAPB0108 for Automatic Identification and Data Capture (AIDC), and ISB0099 for Patient Identifiers for Identity Bands.
HSSIB recommendations
To reduce incidents of patient misidentification, the HSSIB report makes the following recommendations and observations:
- Safety observation O/2024/017: Those purchasing and implementing electronic patient record systems in healthcare organisations can improve patient safety by ensuring those systems are compliant with relevant risk management standards (such as DCB0129, DCB0160 and DCB1077).
- Safety recommendation R/2024/019: HSSIB recommends that NHS England reviews and identifies system-wide requirements for scanning in positive patient identification. This is to support local organisations to use scanning technology to reduce misidentification incidents.
Scan4Safety and point-of-care scanning
The report also refers to comment from NHS England which highlights the potential of Scan4Safety to support patient identification and improve patient safety. This reinforces the ongoing central commitment to Scan4Safety and point-of-care scanning as reflected against priorities outlined in the Digital Clinical Safety Strategy.
GS1 UK continues to work closely with central arm’s length bodies, solution providers (such as EPR providers) and NHS trusts, to support the national adoption of standards for accurate positive patient identification.