March 26, 2026 Opinion piece
Across the NHS, many of the most important safety moments happen almost quietly. A nurse scans a patient’s wristband. The digital record confirms identity. A medicine pack is scanned next. The system checks the product, strength and dose. Batch and expiry information appears instantly and the nurse moves on with confidence.
During the recent Talking Pharmaceuticals podcast, GS1 UK’s Chris Florey and Amna Khan-Patel reflected how fragile manual systems have become amid the growing digital health landscape. NHS teams are reporting rising numbers of medicine packs that arrive without a GS1 DataMatrix or with barcodes that systems cannot read. These inconsistencies are now affecting workflows from pharmacy stores to the patient’s bedside.
Their conversation offered a candid look at why this is happening, what it means for clinical and operational teams and why reliable barcode data is now one of the most important foundations for safe and effective medicines management.
A change in rules with consequences few expected
The discussion opened with the regulatory shift that began on 1 January 2025. Under the Windsor Framework, UK only medicine packs are no longer required to carry a two-dimensional GS1 DataMatrix.

As Chris explained, the change arrived quietly but has sent ripples through the system.
Hospitals that once received uniformly scannable packs now see wide variation in barcode quality. Some packs can be scanned easily. Some require repeated attempts. Others carry nothing a scanner can read.
The result is a growing sense of unpredictability. Pharmacy teams do not know until a delivery arrives whether the stock will pass scanning checks or need to be handled manually. Chris described trusts where staff now check whole batches at the loading bay because they can no longer assume the barcode will work at the point of care.
Real stories from the frontline
Amna spoke openly about the experience of clinical teams when a pack refuses to scan. She described the reality of a busy ward where nurses juggle urgent tasks, anxious families and the need for accuracy under pressure.
In these moments, she said, scanning is meant to feel like support rather than an extra step.
“Scanning should feel like reassurance. It should protect the five rights so that nurses can focus on the patient. When a pack does not scan, you feel the loss of that reassurance immediately. It changes the whole rhythm of the round.”
Amna’s reflection captured a truth that appears again and again across NHS organisations. A missing or unreadable barcode is not a minor technical fault. It is the removal of a safety control that protects patients and supports clinical judgement.
Chris connected this to the wider medicines system. He spoke about his visit to an automated pharmacy hub where teams demonstrated how a single barcode error could halt a run of dispensing. Robots could not recognise the pack. Staff had to remove it, intervene manually and reset the workflow.
“Automation depends on accurate data. The GS1 DataMatrix is the link between the physical pack and the digital system. When that link fails, everything slows and confidence drops.”
Evidence from the MHRA Inspectorate reflects what they described. Recent reports show GTINs scanning as entirely different medicines, missing DataMatrix symbols and incorrect formats that automated systems reject. These issues have led to quarantines, rework, stock discards and added pressure on clinical and pharmacy teams.
Two incidents in 2025 illustrate the point. Multiple batches of fexofenadine tablets were found to carry a barcode that identified a different prescription medicine. The same problem was identified on simvastatin packs the same year. Amna noted that these were not just technical faults. They were moments where a key line of defence failed.
At the bedside, the impact becomes personal
The conversation naturally moved to the point of care. Amna described watching nurses work in organisations that use closed loop medicines administration. Scanning the patient wristband and the pack creates a real time safety check that reduces clinical risk and supports good care.
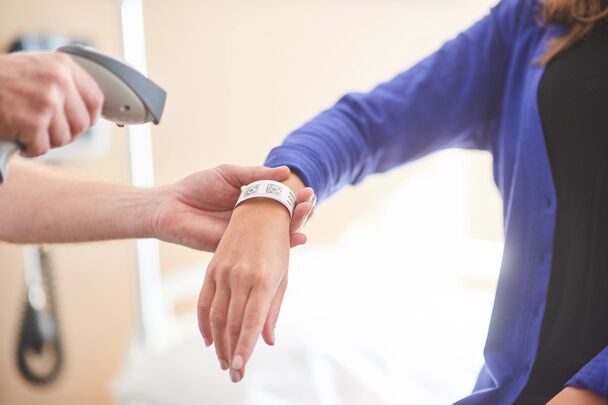
When scanning works, nurses can concentrate fully on the patient. When it fails, they must stop, enter details manually and carry out additional visual checks. These moments can feel small but they introduce avoidable cognitive load and uncertainty. The Patient Safety Commissioner for England has warned that barcode inaccuracies can have severe consequences and may lead to the wrong dose or formulation being given.
Chris added that bedside scanning also plays an essential role in traceability. When a recall is issued, hospitals with reliable scanning can identify affected stock within minutes and act immediately. In trusts where scanning is incomplete or inconsistent, recalls can take days and require extensive manual searching.
Scan4Safety demonstrator sites have shown that consistent scanning can reduce recall completion times from more than a week to under an hour.
A system beginning to raise its voice
Chris and Amna’s experiences reflect a wider national concern. Community pharmacists are also reporting rising numbers of inconsistent barcodes. Some have seen duplicated GTINs across manufacturers, making every scan a cause for caution rather than confidence. Professional bodies have urged the MHRA to require consistent use of two-dimensional barcodes and accurate product information to protect both patients and staff.
The Royal Pharmaceutical Society has echoed these calls, highlighting that two-dimensional barcodes are essential for medicines safety and that their absence is creating challenges across all areas of care.
Amna reflected on this growing movement during the podcast.
“People often talk about digital transformation as if it is about new technology. The truth is that everything depends on the identifier on the pack. If that is not right, nothing else works as it should.”
A way forward that strengthens the whole system
Toward the end of the conversation, Chris spoke about the direction of national policy. The House of Lords Public Services Committee has recommended that two-dimensional barcodes be mandated on all UK medicine packs to improve traceability, strengthen stock visibility and reduce the risk of avoidable harm. GS1 UK supports this recommendation and continues to work closely with NHS England, manufacturers and regulators to help rebuild consistency across the supply chain.
As the podcast drew to a close, Chris offered a final thought that captured the essence of the conversation.
“The medicines pathway is a chain. It only works when every link is strong. Accurate barcodes keep the chain connected from manufacturer to patient.”
Amna then shared a closing reflection that brought the discussion back to those quiet moments of care.
“In the end, every scan is about safety. It is about making sure each patient gets exactly what they need. This is why consistency matters.”



